Male Breast Cancer
Overview
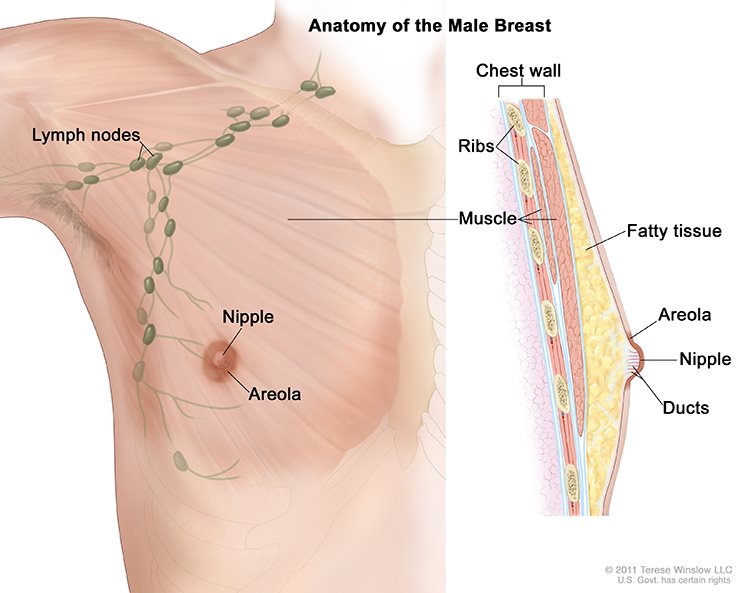
A man’s breast contains glandular tissue, the cells of which can develop into a malignant tumor. Males are less likely to develop breast cancer than females because their breast ducts are less developed, and they have less of the female hormones that impact breast cell growth. Cancer cells in the breast can spread to the lymph nodes via the lymphatic vessels and become increasingly dangerous. Infiltrating ductal carcinoma is the most common form of breast cancer found in men, and men typically present with more advanced disease than women due to late detection. This is why awareness among men is very important.
Statistics
- In 2024, there will be an estimated 2,790 new cases of invasive male breast cancer diagnosed, and an estimated 530 men will die of the disease in the United States.
- In Texas, an estimated 186 men will be diagnosed with breast cancer in 2024, with an estimated 36 deaths.
- Male breast cancer accounts for less than 1% of all breast cancer diagnoses.
- One in 726 men will be diagnosed with breast cancer in his lifetime.
- Outlook for survival by stage from breast cancer in men and women is about the same. However, male breast cancer is frequently diagnosed at a later stage when it is more difficult to treat.
- A family history of breast cancer can increase a man’s risk of breast cancer. Men with a mutation of the BRCA2 gene have a lifetime breast cancer risk of around 6%. The BRCA1 gene in men is responsible for a 1% lifetime risk of breast cancer.
Risk Factors
- Age: As men age, their risk of developing breast cancer increases, with most male breast cancers detected between 60 and 70 years old.
- Radiation: Men who have been treated with radiation around the chest area have an increased risk of breast cancer.
- Family History: Men with close blood relatives who have breast cancer or who have a mutation of the BRCA1 or BRCA2 gene face an increased risk. Men with a strong family history of breast cancer should consider genetic testing to determine if they have the gene mutation, which could impact their risk both as a patient and carrier.
- Estrogen: Males with higher levels of estrogen due to diseases, such as the genetic disorder Klinefelter syndrome, have an increased risk. Also, men taking estrogen-related drugs for hormone therapy or sex changes may be at an increased risk.
- Alcohol: Men who are heavy drinkers face an increased risk because alcohol toxicity causes liver diseases, like cirrhosis, which can cause higher estrogen levels.
- Obesity: Just like with women, obesity can contribute to breast cancer in men. Obese men have higher levels of estrogen because fat cells convert male hormones known as androgens to estrogen.
- Testicular Conditions: Risk of developing male breast cancer can be increased by certain testicular conditions, such as an undescended testicle, testicle removal, and adult mumps.
Symptoms
As with women, early detection of breast cancer is crucial to treatment and survival. Men with a family history, such as immediate family members with breast cancer, or a BRCA mutation, should discuss how to manage risk with their physician. Signs to look for include:
- Redness or scaliness on the breast skin and around the nipple
- A nipple that turns inward
- Nipple discharge, including blood
- A lump or swelling in the chest or underarm area, typically without pain
- Puckering or dimpling skin
- Skin that looks like orange peel
- Change in the size or shape of the breast
Treatment Options
Because so few men are diagnosed with breast cancer, it is difficult to study the treatment of breast cancer in men separately from women. Treatment of breast cancer in men is similar to treatment for women with the disease. Treatment options can include surgery, radiation, chemotherapy, hormone therapy, targeted therapy, immunotherapy, proton therapy, and palliative medicine. A combination of treatments may be used to provide the best chance of disease control.
Sources: American Cancer Society, Centers for Disease Control and Prevention, National Cancer Institute, National Center for Biotechnology Information, Texas Cancer Registry, and Texas Center for Proton Therapy